
CPR Resource Center
The most comprehensive library of emergency training resources — including videos, articles, downloads, and more.


The most comprehensive library of emergency training resources — including videos, articles, downloads, and more.
Part I of our series discussed the recognition of cardiac arrest and getting help. We’ll now discuss bystander initiated CPR and the obstacles that prevent CPR from being started immediately. This will lead us into Part III – Public Access to Defibrillation which will discuss use of an automated external defibrillator (AED) and deployment strategies.
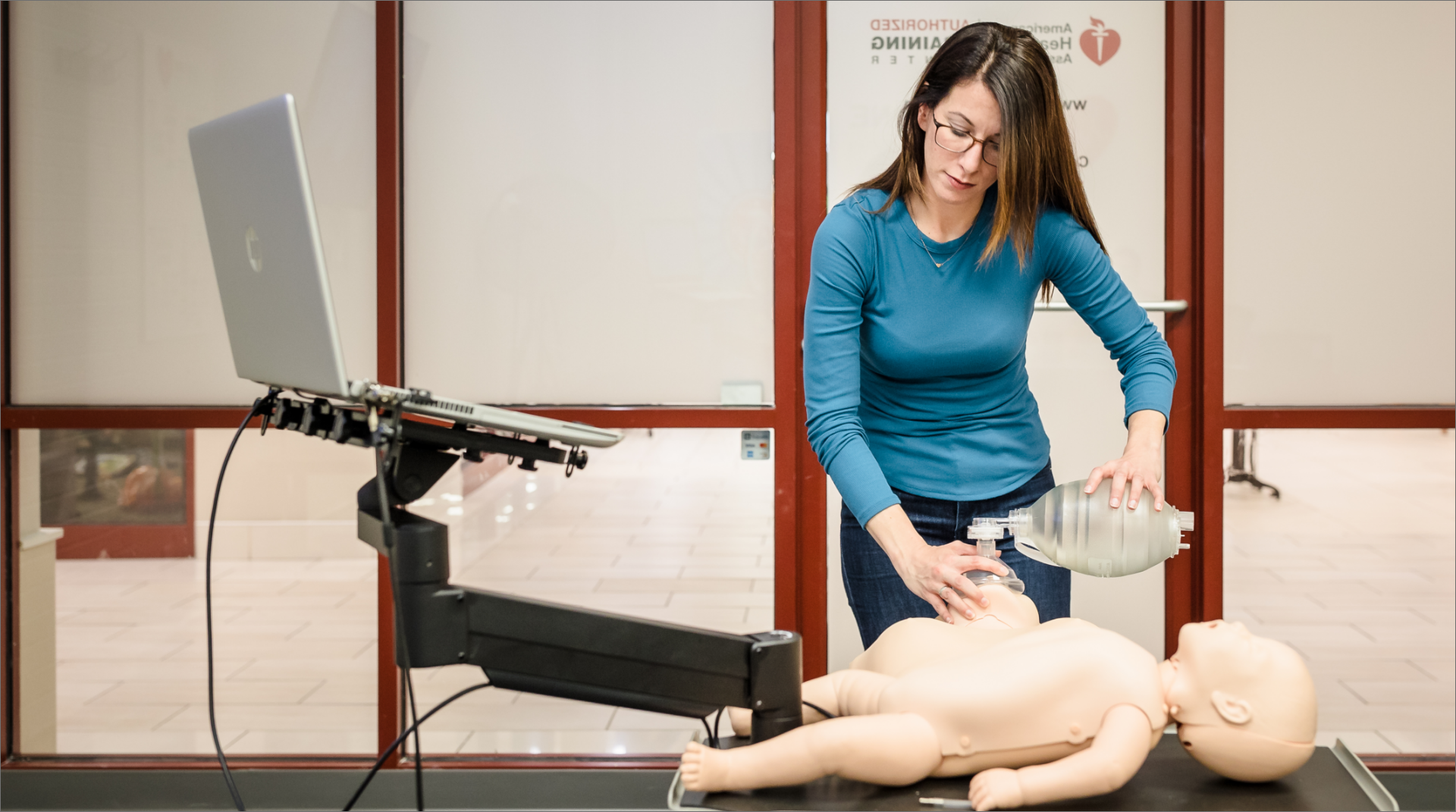
When cardiac arrest occurs in the public setting, it should be assumed that bystanders will not be carrying pocket masks and breathing barriers on their person. Keychain pocket masks provide convenient personal protection for delivering rescue breaths, but most trained rescuers do not even carry these. Bystanders and healthcare providers are not expected to provide mouth to mouth resuscitation.
A. Hands Only CPR. Hands only CPR provides chest compressions to victims of cardiac arrest victim. A bystander that finds a person who is not responsive and is not breathing normally should call 911, request an AED, and start Hands Only CPR.
Is the person responsive? NO
Is the person breathing normally? NO
We are going to start CPR. GO
The first two actions of calling 911 and retrieving an AED should be delegated to another bystander if someone else is nearby. Be sure to specify the bystander that will complete these actions. If you’re alone, call 911 and retrieve the AED first before providing care.
To provide hands-only CPR, remove clothing to bare the person’s chest.
Interlock your fingers and place the heel of your hand on the lower half of the breastbone, in-line with the nipples.
Lock your elbows and use your body weight to compress the chest about two inches. Repeat at a rate of 100 compressions per minute (the same tempo as Staying Alive by the Bee Gees or your choice of another CPR song).
If other bystanders are available, rotate rescuers every two minutes.
Continue providing hands-only CPR until trained help arrives and takes over. If the person begins to breathe normally or have meaningful movement, stop chest compressions and watch them until help arrives. Be prepared to start chest compressions again if they stop breathing normally.
Here are the important notes to remember for providing high-quality hands only CPR:
PUSH HARD: Compress the chest two inches. Allow full chest recoil – there should be no pressure on the chest between each compression.
PUSH FAST: Compress the chest at a rate of 100 compressions per minute. Avoid pushing too fast (over 120 compressions per minute).
MIND THE GAP: Gaps in chest compressions kill people. Avoid any interruptions in CPR. Count down when switching rescuers so the next rescuer can start without missing a beat. The rescuer using the AED can also apply the pads while the rescuer is still providing chest compressions.
The Cardiac Arrest Registry to Enhance Survival (CARES) collects data on cardiac arrest victims provided by 1,400 EMS providers and 1,900 hospitals nationwide. This collaboration provides a snapshot of cardiac arrest incidence, implementation of chain of survival steps, and patient outcomes. The reports can provide a comparison for how a particular community, state, or region performs in these metrics.
The most pertinent figures to consider when evaluating the frequency of bystander initiated CPR include whether or not the cardiac arrest was witnessed and whether or not bystanders initiated CPR before EMS arrived.
In 2017, approximately 49% of cardiac arrests reported to CARES were witnessed. Of these witnessed cardiac arrests, only 38% received bystander initiated CPR and only 11% of public cardiac arrests had an AED applied.
When we talk about the low rates of bystander initiated CPR, it is important for us to recognize the obstacles that bar people from acting:
Learn or review skills now and regularly so that you’re ready in an emergency. You can learn Hands-Only CPR from the AHA or become certified in CPR at a Heartsaver CPR AED course.
Part III of our series will discuss the use of Automated External Defibrillators in cardiac arrest and deployment strategies.
Help Me Find a Course