
CPR Resource Center
The most comprehensive library of emergency training resources — including videos, articles, downloads, and more.


The most comprehensive library of emergency training resources — including videos, articles, downloads, and more.
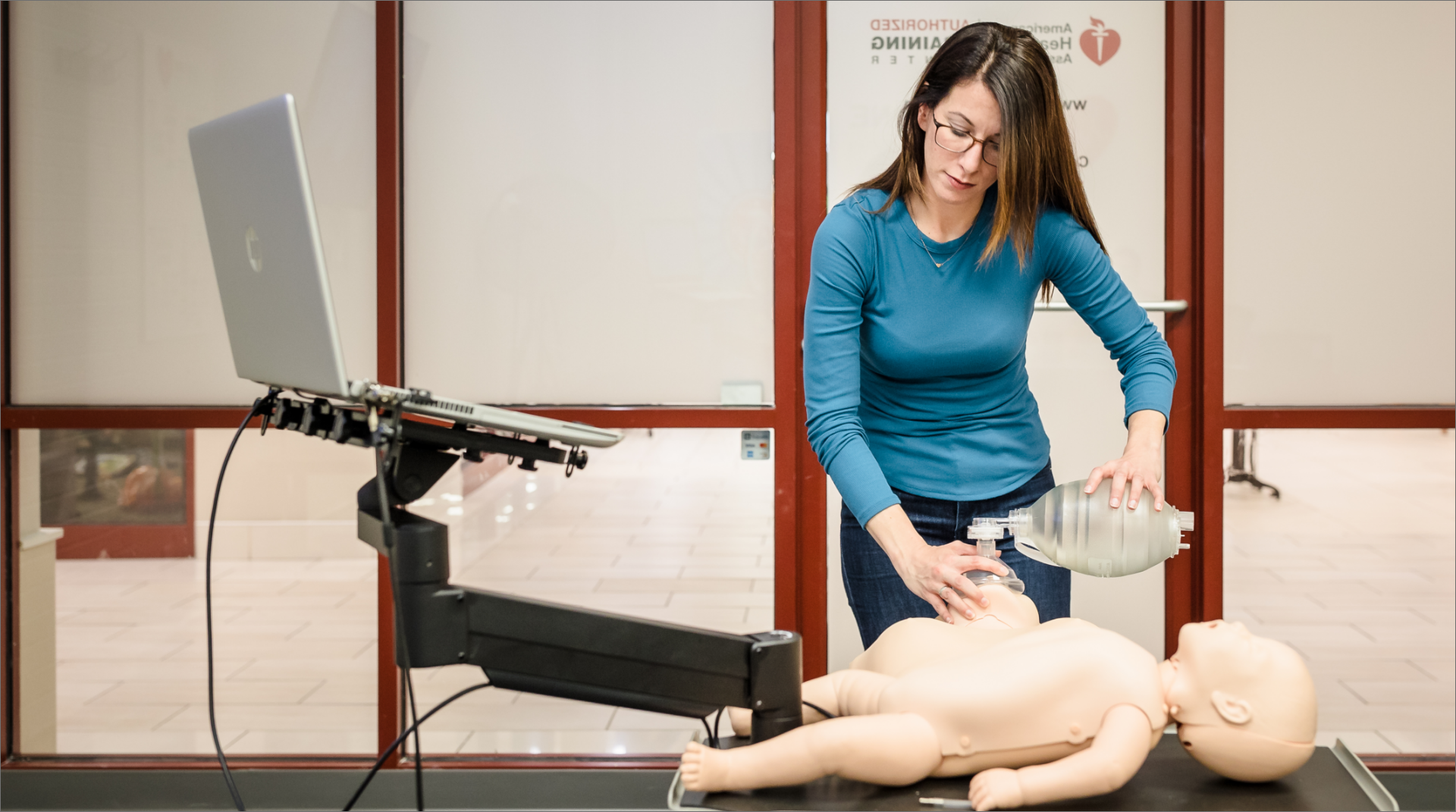
During the many stages of our journey as healthcare providers, we train to use many different tools. Early in my career one of the tools I first learned to use was the bag valve mask (BVM). The operation of the device itself is pretty simple. It’s important, however, to not let the ease of a mechanical skill itself bely the importance of the role it plays in a successful resuscitation effort.
Think about this – if you need to use a BVM for your patient, you can take one thing as a given: autonomic function is impaired in some way. If one of a patient’s autonomic functions such as respiration are impaired, logic dictates a couple of things. One of the body’s natural “safeguards” such as the stretch reflex in the lungs that prevents us from taking too large of breath also is not functioning properly. We, as a necessity, interfere with that simple air going in and out process. Done correctly, it’s a good thing, a necessary and lifesaving action.
As BVM use requires constant repeated operation by an individual(s), there’s no consistency in tidal volume delivery or respiratory rate. With every squeeze of the bag the rescuer is actually unknowingly selecting the volume delivery as well as the rate1. Furthermore, practicing BVM use or CPR does not ensure operators are learning proper techniques if they are not afforded both feedback and the opportunity to correct their techniques2 in a controlled environment. With any skill, we tire and fatigue over time and thus become less accurate or effective at a skill. Even though the American Heart Association (AHA) recommends switching compressor and ventilator roles every two minutes, it like all algorithms, is a guideline and not an absolute.
In any resuscitation effort, it’s not uncommon for one’s adrenaline to be elevated thus our perception of time may not be accurate. Waiting six seconds between breaths can feel like an eternity. Performed incorrectly, BVM ventilation can accelerate hypoxia and accelerate the airway obstruction that naturally occurs during profoundly decreased levels of consciousness3. During the decompression phase of CPR, hyperventilation will result in high intrathoracic pressure. If we ventilate at an excessive rate (hyperventilate) or with excessive volume, too much of that positive pressure builds up. Left unrelieved, a pneumothorax could result. Consequently, cardiac pre-load and output are decreased due to excessive pressure on the great vessels. Reduced pre-load results in lower stroke volume and ultimately decreased cardiac output1,4. All ingredients for a failed resuscitative effort.
Patients with Chronic Obstructive Pulmonary Disease (COPD) already have lung function compromise due to damaged anatomy. Those alveoli that are already poorly functioning due that reduced elasticity can’t handle their share of the “respiratory workload”. As such, the healthy ones have to “pick up the slack” in addition to handling their own workload. This extra burden stresses the healthy alveoli which can put them at risk of rupture5. Surfactant breakdown commonly occurs, resulting in the lungs not being able to stay inflated properly. Therefore, less alveolar-capillary membrane gas exchange. Hyperventilating or over ventilating worsens these processes.
These limitations are not isolated to lung or heart disease. Hyperventilation with a BVM can negatively affect stroke patients in several ways. A severely brain-damaged patient is likely unable to protect his/her airway. Unbalanced blood gas levels cause cerebral vasoconstriction. The less blood flow to tissues suffering insult, the slower healing occurs or the lesser the possibility thereof.
As with hyperoxia, there’s excessive O2 in the organs/tissues of the body. Oxygen toxicity occurs when tissues are inundated with excess oxygen much greater than is normally breathed and what is needed by damaged tissues. We commonly see oxygen toxicity defined as acute (high concentrations of oxygen for a short duration) and chronic (lower concentrations of oxygen for a longer duration)7. The lowest possible concentration of oxygen that alleviates tissue hypoxia is optimal in all patients, especially those with Acute Respiratory Distress Syndrome (ARDS)7. Metabolic issues like blood gas levels and hyperoxia in stroke patients can be more complex. Management is best handled in the ED or ICU where blood gas sampling can be monitored. In the field, pulse oximetry and end-tidal capnography are acceptable with the end goal always being transport to a medical facility.
The good news is that a properly trained provider can mitigate these hazards. User error is the most common, and remains the most correctible.
Fortunately, the AHA has provided some great guidance for how we as providers can reduce hyperventilation; through following their “Recommendations for Fundamentals of Ventilation During Cardiac Arrest”. By monitoring the volume of air we deliver with a BVM, capping that amount as we see the chest rise (level 2A evidence), and ensuring consistent 1-second delivery of every rescue breath or ventilation during CPR (level 2B evidence), we as practitioners can reduce the potential for harm8. Of course, not everyone can do a picture-perfect C-E grip with a BVM. As long as you have the proper amount of air going WHERE it is supposed to WHEN it is supposed to, hand positioning doesn’t have to be fancy. It just has to work.
When it comes time to educate others on how to prevent hyperventilation during classes, in addition to stating the AHA evidence, instructors should be monitoring the rate and volume of breaths delivered by students. A trained provider should practice and ensure adequate face-to-mask seal and take the time to count out loud or in the head the 6 second count recommended during assisted ventilations. If the mask has noisy air leaks with chest rise, the pressure is likely far too high. If there is adequate chest rise and no air leaks, the pressures are much more likely to be safe in the resuscitation period. The goal should be to squeeze until chest rise is visible, but not pronounced or with mask air leaking audibly. Many BVMs have a PEEP measuring device from 1-10, a PEEP (air pressure at the end of exhalation within the lungs) of 6-8 is ideal to prevent injury to lungs that could result from excess pressure. Like started at the beginning of the article, ensuring proper technique through timely positive and critical feedback is the gateway to success and keeping our patient’s lungs out of trouble.
The author would like to thank the following for their time & suggestions in review:
Help Me Find a Course